Radiculopathy is a condition where one or more of the nerves in your spine become damaged causing pain. If the nerve that is being irritated is in your neck, also known as cervical radiculopathy, you may experience symptoms in your neck and possibly down your arm(s). If it is in your low back (lumbar radiculopathy), you may experience symptoms in your low back and down your leg(s). Less commonly, this can occur in your midback (thoracic radiculopathy) which would cause you to have symptom in your midback and across your chest and/or abdomen. The symptoms you may experience include:
pain, numbness, tingling, weakness in the affected area. At times, the symptoms you experience may follow a particular pattern also known as a dermatome (See Fig.1).
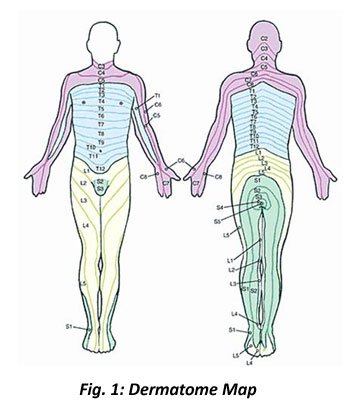
This can help determine the specific level of the spine that is irritating the nerve causing your symptoms. This can allow for targeted treatment which can potentially give you better treatment results.
Commonly lumbar radiculopathy is used interchangeably with sciatica. Think of lumbar radiculopathy as a more specific form of sciatica and that sciatica is generally meant as any type of leg pain that originates from irritation of the sciatic nerve. It is important to differentiate the level at which the nerve pain is coming from as this will determine your course of treatment.
Radiculopathy can be acute or chronic. Acute radiculopathy typically occurs after a disc in your spine herniates, compressing one or more nerves in your spine. This causes the nerve(s) to become inflamed causing the symptoms you experience. Other possible factors that could be contributing and/or causing the nerve irritation is a bone spur that presses on the nerve, misalignment of your spine that pinches the nerve, or a tear in the disc that does not physically compress the nerve(s) but chemically irritates it. Other less common causes of radiculopathy include tumors, infections or vasculitis. Chronic radiculopathy occurs when your symptoms continue to persist through time, usually more than 3 months.
Treatment for this condition should be tailored to addressing the specific nerve(s) that are being irritated. Medication management and physical therapy are the usual first line treatments. If your symptoms persist, it is important to be evaluated by a spine specialist as soon as possible. In most cases, surgery is not an option especially in the acute phase. As the longer you wait to get specific treatment for your pain the higher the likelihood of this being a lifelong problem, it may be in your best interest to not wait to be seen by a spine surgeon. In addition, understanding that in a large majority of cases, surgery is not an initial option and/or you may not be a candidate for surgery or you might not even want surgery, your initial consultation with a spine surgeon will likely lead to another referral to an interventional spine specialist. The time you wait to see a surgeon to only be referred to another specialist is time lost in appropriately treating your pain.
If your symptoms do not resolve in a week or so, you may be a candidate for a targeted procedure to not only diagnose but treat your pain (see transforaminal epidural steroid injection). An MRI is not needed in most cases before a procedure is done as your symptoms dictate where the injection is being performed. This is determined after your initial evaluation by a spine specialist.
Surgery typically becomes an option only after you have failed conservative measures including interventional treatments. This is the time where a spine surgical evaluation is the most valuable for you as well as the surgeon. Here, you can specifically discuss the surgical options and the potentially need for further studies especially if the cause of your pain is still unclear. However, after being evaluated by a spine specialist initially prior to your surgical evaluation, the visit with your surgeon will be much more informative as all diagnostic tests and nonsurgical treatment options have been pursued. If surgery is not an option to help control your pain, other more advanced minimally invasive surgeries may help decrease your pain by >50% without the use of oral “pain” medications. (see spinal cord stimulation and intrathecal drug delivery systems)